Information about MyHumana
App Feature
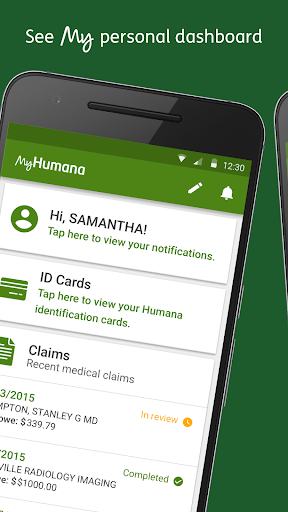
MyHumana centralizes Humana insurance management: view coverage details and deductibles, access and share digital ID cards, check drug pricing, review claims, find in‑network providers via GPS, manage premium payments (including recurring), and edit profile details. It also highlights wellness tracking and personalized recommendations for a more integrated health experience.
Verdict
Verdict: A reliable, feature‑complete insurance companion for Humana members, best if you want quick access to coverage, claims, and ID cards on the go.
Who is it for
Best for:
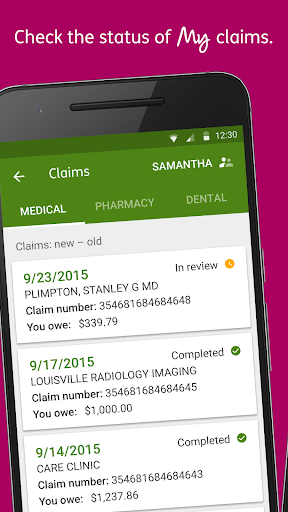
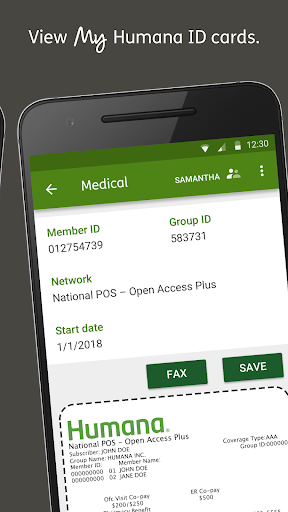
- Humana members who need fast access to ID cards, coverage, and claims
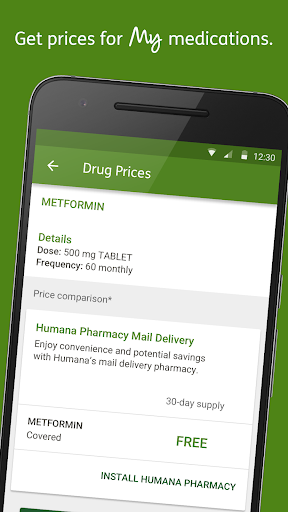
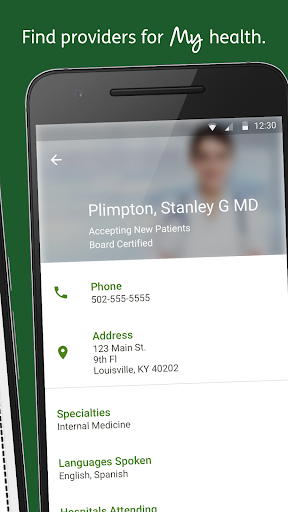
- Users who want in‑network provider search and drug price comparisons
- Members managing premium payments or dependents from one app
Not ideal for:
- Non‑Humana users seeking general health or fitness apps
- Power users wanting deep medical records interoperability beyond insurance data
- Privacy‑sensitive users who avoid location permissions for provider search
Real-world User Experience
Users like it:
Overall strong ratings (4.3 with thousands of reviews) suggest users value the convenience of digital ID cards, quick visibility into benefits and claims, accurate provider search, and straightforward premium payment tools.
Users complain about:
Some users likely encounter occasional login or authentication friction, intermittent performance hiccups, and limitations on editable profile fields; GPS-based search may impact battery when left on.
Is it Worth Paying For?
The app is free with no ads or in‑app purchases; for Humana members, the value is high at no cost.
How it Compares to Alternatives
Compared with other insurer apps (e.g., UnitedHealthcare, Aetna Health, BCBS, Cigna), MyHumana covers the expected basics—benefits, claims, digital IDs, provider search—and stands out with integrated drug pricing and robust payment options. Some competitors offer broader health integrations or telehealth shortcuts; MyHumana emphasizes insurance workflows and adds wellness tracking, but its utility largely depends on being a Humana member.
Summary
MyHumana delivers a practical, all‑in‑one portal for Humana members to manage insurance essentials: coverage details, claims, ID cards, provider discovery, drug pricing, and payments. Its clean feature set reduces the need to call support or log into a desktop portal, while wellness tracking adds a light health layer. Ratings indicate dependable day‑to‑day use, though users may face occasional login or performance bumps and must enable location for the best provider search experience. If you’re insured by Humana, this free, ad‑free app meaningfully streamlines routine tasks and puts key plan information at your fingertips.
Ratings
Trending APP












Alternative to this app